-
Address:
17888 67th Court North
Loxahatchee, FL
-
Mail us:
contact@wrightacademia.org
- submit manuscript
Table of content
Editorial |
Open Access |
Volume 2 | Issue 1 |
Coronavirus-19, Monocyte/Macrophage Glycolysis and Inhibition by Melatonin
Russel J Reiter, PhD1, Ramaswamy Sharma, PhD1, Rafael Castillo, MD2, Paul E Marik, MD3, Alberto Dominguez Rodriguez, MD4, Daniel P Cardinali, MD5 and Jan Tesarik, MD, PhD6
1Department of Cell Systems and Anatomy, UT Health San Antonio, USA
2FAME Leaders' Academy, FAME Executive and Editorial Offices, Philippines
3Department of Internal Medicine Chief, Pulmonary and Critical Care Medicine, Eastern Virginia Medical School, USA
4Departamento de Cardiología, Hospital Universitario de Canarias, San Cristóbal de La Laguna, Spain
5Faculty of Medical Sciences, Pontifica Universidad Catolica Argentina, Argentina
6MAR Gen Clinic, Spain
*Corresponding author: Jan Tesarik, MD, PhD, MAR Gen Clinic, Camino de Ronda 2, 18006 Granada, Spain, E-mail: jtesarik@clinicamargen.com
Citation: Reiter RJ, Sharma R, Castillo R, Marik PE, Rodriguez AD, et al. (2021) Coronavirus-19, Monocyte/Macrophage Glycolysis and Inhibition by Melatonin. J SARS-CoV-2 COVID 2:007.
Copyright © Reiter RJ, et al.
Received: |
Accepted: |
Published: |
Two highly relevant studies related to SARS-CoV-2 and coronavirus disease (COVID-19) and supporting the use of melatonin to prevent and treat this serious infection were published recently. Campos-Codo and colleagues [1] documented experimentally their claim that drugs which specifically target hypoxia inducible factor-1α (HIF-1α) would likely have great therapeutic value in treating COVID-19. The second report is a retrospective analysis based on the clinical experience at the Columbia University Irving Medical Center with the use of drugs to treat respiratory distress in COVID-19-infected patients who required endotracheal intubation [2].
Hyperinflammatory monocytes/macrophages accumulate in abundance in the lower respiratory tract where they play a key role in determining the severity of SARS-CoV-2 infections. Campos-Codo, et al. [1] found that monocytes/macrophages infected with the SARS-CoV-2 virus reprogram their metabolism from the conventional mitochondrial oxidative phosphorylation (OXPHOS) to the (usually) pathological cytosolic glycolysis. This so-called Warburg-type metabolism is aided by the inadequately controlled elevated blood glucose levels of diabetic patients, which enhances cellular glycolysis, viral replication and hastens development of a severe respiratory infection resulting from the elevated cytokine release ("cytokine storm"). Thus, diabetes is a risk factor for the progression and prognosis of COVID-19. In the more recent report, after a comprehensive evaluation of 791 patients diagnosed with COVID-19 who required tracheal intubation, Ramlall, et al. [2] found melatonin to be the only drug that was statistically associated with higher positive clinical outcome including survival of patients intubated and in those requiring mechanical ventilation.
Mechanistically, Campos-Codo and coworkers [1] noted that glycolysis was a result of the increased generation of mitochondrial reactive oxygen species (mtROS) in the virus-infected cells. In turn, the amplified mtROS stabilized HIF-1α, a potent stimulator of pyruvate dehydrogenase kinase (PDK) which inhibits pyruvate dehydrogenase (PDH) thereby preventing the glucose metabolite, pyruvate, from being metabolized to acetyl-coenzyme A in the mitochondria. This causes metabolic reprogramming by shifting pyruvate metabolism to the cytosol, decreasing OXPHOS and augmenting mtROS. Monocytes/macrophages functioning with this metabolic phenotype produce more cytokines leading to T cell destruction and killing of the alveolar lining cells, thereby severely aggravating the COVID-19 infection. Campos-Codo, et al. [1] concluded that "targeting HIF-1α may have great therapeutic potential for the development of novel drugs to treat COVID-19".
Many reports suggested the use of melatonin to treat COVID-19 disease, [3-6] and in the studies where it has been tested for this purpose, melatonin has proven highly effective [7]. The rationale for melatonin use as a treatment for COVID-19 stems from is ability to inhibit other viral infections [8]. Also, melatonin is likely to convert highly pro-inflammatory glycolytic M1 macrophages to anti-inflammatory M2 macrophages which utilize OXPHOS [9]. Melatonin reprograms cytosolic glycolysis to mitochondrial OXPHOS because it down-regulates HIF-1α, which leads to PDH disinhibition, [10,11] causing the mitochondrial metabolism of pyruvate, stimulation of the tricarboxylic acid cycle, improved OXPHOS and reduced mtROS. In addition to reducing mtROS generation under these conditions, melatonin and its metabolites are highly effective direct scavengers of partially reduced derivatives of oxygen [12]. Melatonin works via the precise mechanism proposed by Campos Codo, et al. [1] for drug targeting of COVID-19. Moreover, beyond its action as an immunomodulatory agent, there is evidence that melatonin can act to reduce the viral load by inhibiting the epidermal growth factor receptor signaling, a requirement for virus replication [13]. The multiple actions of melatonin in inhibiting the progress of a SARS-CoV-2 infection are summarized in the (Figure 1). Considering the large amount of experimental/clinical data related to the high efficacy of melatonin in inhibiting viral infections including SARS-CoV-2, [14-17] we strongly urge the use of melatonin for the prevention and treatment of COVID-19 infection.
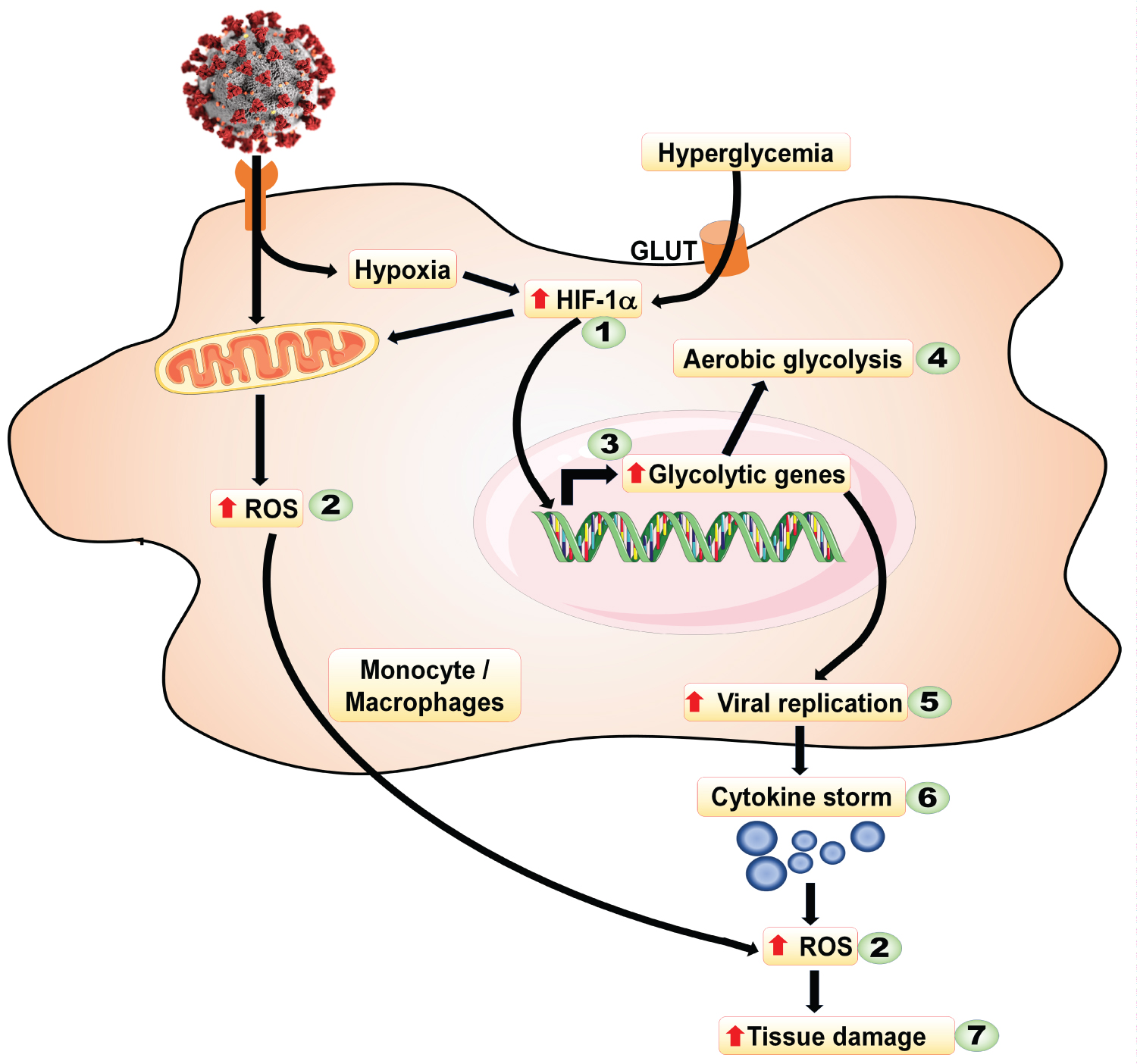
Figure 1: Metabolic events involved in hyperglycemia-mediated exaggeration of the cytokine storm in SARS-CoV-2 infected pro-inflammatory macrophages. Melatonin's ability to reduce the molecular processes associated with the cytokine storm is identified and includes: 1) Inhibition of HIF-1α; 2) Scavenging of ROS; 3) Reducing glycolytic enzymes; 4) Preventing aerobic glycolysis; 5) Inhibiting viral replication; 6) Limiting the pro-inflammatory cytokine storm; 7) Reducing tissue damage. Each of these actions has been documented in experimental studies and are likely occur in SARS-CoV-2 infected individuals, whether or not they also suffer from diabetes. The associated references are cited in the text.
ACE2: Angiotensin converting enzyme 2; GLUT: Glucose transporter; ROS: Reactive oxygen species.
The risk of individuals developing an overt or lethal COVID-19 infection is also consistent with what is known about endogenous melatonin levels throughout life. Nocturnal melatonin titers are highest in children and wane throughout life such that the molecule is significantly depressed in the elderly, [18] the age at which COVID-19 infections are worse [19]. There are also individuals who suffer from genetically-determined hypomelatoninemia even at an early age; these individuals may also be at increased risk of a serious COVID-19 infection.
Melatonin is a commonly-used sleep aid. In critically-ill patients, melatonin improves sleep and wellbeing [20] both of which would also be beneficial to SARS-CoV-2 infected patients. Melatonin has an uncommonly-high safety profile, [21] is inexpensive, is stable without refrigeration and would be particularly useful in underdeveloped countries lacking easily accessible or high-quality health care. Because of melatonin's metabolic reprogramming actions, etc., it is a worthy candidate for further testing and consideration as a treatment of COVID-19, especially since Ramlall, et al. [2] reported the elevated ability of melatonin as an efficacious treatment in intubated and mechanically-ventilated COVID-19 patients. Moreover, Castillo, et al. [7] have shown that the outcome of COVID-19 infected patients is improved as a result of melatonin treatment.
Declaration of Interests
The authors declare none.
References
- Campos-Codo A, Davanzo GG, Monteiro LB, et al. (2020) Elevated glucose levels favor SARS-CoV-2 infection and monocyte response through a HIF-1α/glycolysis-dependent pathway. Cell Metab 32: 437-446.
- Ramlall V, Zucker J, Tatonetti N (2020) Melatonin is significantly associated with survival of intubated COVID-19 patients. Med Rxiv.
- Acuña Castroviejo D, Escames G, Figueira JC, et al. (2020) Clinical trial to test the efficacy of melatonin in COVID-19. J Pineal Res 69: e12683.
- Cardinali DP (2020) High doses of melatonin as a potential therapeutic tool for the neurological sequels of covid-19 infection. Melatonin Res 3: 311-317.
- Dominguez Rodriguez A, Abreu Gonzalez P, Marik PE, et al. (2020) Melatonin, cardiovascular disease and COVID-19: A potential therapeutic strategy? Melatonin Res 3: 318-321.
- Reiter RJ, Abreu-Gonzalez P, Marek P, et al. (2020) Therapeutic algorithm for use of melatonin in patients with COVID-19. Front Med 7: 226.
- Castillo RR, Quizon GRA, Juco MJM, et al. (2020) Melatonin as adjuvant treatment for coronavirus disease 2019 pneumonia patients requiring hospitalization (MAC-19 PRO): A case series. Melatonin Res 3: 297-310.
- Anderson G, Reiter RJ (2020) Melatonin: Roles in influenza, COVID-19 and other viral infections. Rev Med Virol 30: e 2109.
- Reiter RJ, Sharma R, Ma Q, et al. (2020) Plasticity of glucose metabolism in activated immune cells: Advantages for melatonin inhibition of COVID-19 disease. Melatonin Res 3: 362-379.
- He M, Zhou C, Lu Y, et al. (2020) Melatonin antagonizes nickel-induced aerobic glycolysis by blocking ROS-mediated HIF-1alpha/miRNA)/ISCU axis activation. Oxid Med Cell Longev 2020: 406284.
- Reiter RJ, Sharma R, Rosales-Corral SA (2021) Anti-Warburg effect of melatonin: A proposed mechanism to explain its inhibition of multiple diseases. Int J Mo Sci 22: 764.
- Galano A, Reiter RJ (2018) Melatonin and its metabolites vs oxidative stress: From individual actions to collective protection. J Pineal Res 65: e12514.
- Tesarik J (2020) Melatonin attenuates growth factor receptor signaling required for SARS-CoV-2-replication. Melatonin Res 3: 534-537.
- Zhong R, Wang X, Ni L, et al. (2020) COVID-19: Melatonin as a potential adjuvant treatment. Life Sci 250: 117583.
- Loh D (2020) The potential of melatonin in the prevention and attenuation of oxidative hemolysis and myocardial injury from cd147 SARS-CoV-2 spike protein receptor binding. Melatonin Res 3: 380-416.
- Brusco LI, Cruz P, Cangas AV, et al. (2021) Efficacy of melatonin in non-intensive care unit patients with COVID-19 pneumonia and sleep dysregulation. Melatonin Res 3: 173-188.
- Gurunathan S, Kang MH, Choi Y, et al. (2020) Melatonin: A potential therapeutic agent against COVID-19. Melatonin Res 4: 30-69.
- Sack RL, Lewy AJ, Erb DL, et al. (1986) Human melatonin production decreases with age. J Pineal Res 3: 406-410.
- García IG, Rodriguez-Rubio M, Mariblanca AR, et al. (2020) A randomized multicenter clinical trial to evaluate the efficacy of melatonin in the prophylaxis of SARS-CoV-2 infection in high-risk contacts (MeCOVID Trial): A structured summary of a study protocol for a randomised controlled trial. Trials 21: 466.
- Cardinali DP (2021) Melatoninand healthy aging. Vitam Horm 115: 67-88.
- Andersen LP, Gögenur I, Rosenberg J, et al. (2016) The safetyof melatonin in humans. Clin Drug Investig 36: 169-175.
INDEXING
PARTNERS








