-
Address:
17888 67th Court North
Loxahatchee, FL
-
Mail us:
contact@wrightacademia.org
- submit manuscript
Table of content
Research Article |
Open Access |
Volume 3 | Issue 1 |
Chest Pain Disposition Practice in a Developing Country: Comparison of a Conservative Method to the HEART Score Method
Mandreker Bahall1*, George Legall1 and Robin Sinanan2
1School of Medicine, Faculty of Medical Sciences, University of the West Indies, Eric Williams Medical Sciences Complex, Mt. Hope, Trinidad, Trinidad and Tobago
2San Fernando General Hospital, Chancery Lane, San Fernando, Trinidad and Tobago
*Corresponding author: Mandreker Bahall, School of Medicine, Faculty of Medical Sciences, University of the West Indies, House #57 LP 62, Calcutta Road Number 3, McBean, Couva, Trinidad, Trinidad and Tobago, Tel: 1-868-763-6608, Fax: 1-868-679-0816, E-mail: vmandrakes@hotmail.com
Citation: Bahall M, Legall G, Sinanan R (2021) Chest Pain Disposition Practice in a Developing Country: Comparison of a Conservative Method to the HEART Score Method. Cardiol Cases Syst Rev 3:010.
Copyright © 2021 Bahall M, et al.
Received: |
Accepted: |
Published: |
Background: Chest pain, associated with diverse aetiologies and management strategies, is a common diagnostic challenge in the emergency department (ED). This study aimed to compare dispatch based on current disposition practices after ED diagnosis with expected disposition as determined by patient history, electrocardiogram, age, risk factors, and tropon in level (HEART) scores.
Methods: The target population comprised all patients presenting with chest pain at the ED at a single centre from May to August 2015. Data were collected from face-to-face interviews. HEART scores were calculated according to the ED protocol for chest pain patients. For the analysis, the outcome variable was the clinical decision to dispatch the patient home or a treatment ward, and for early invasive strategies and was compared to the outcome based on the HEART score. The HEART score (varying from 0 to 10) was calculated by the sum of the individual scores of each variable which is scored 0, 1, or 2. Inferential data analysis included chi-square tests, Mc Nemar tests for paired proportions, and analysis of variance (ANOVA).
Results: The patients (n = 1092) were predominantly female (n = 512; 52.7%), Indo-Trinbagonian (n = 580; 58.9%), and aged ≥ 65 years (n = 265; 26.9%). Acute coronary syndrome (ACS) was absent in > 50% patients (n = 577, 58.6%). There were no differences in ED diagnoses according to sex, age, orethnicity. HEART scores increased with age and ranged from 0 (n = 114; 11.6%) to 8 (n = 2; 0.2%) with a mean equal to 2.70 ± 1.721, with both modal and median scores of 3 (n = 199; 20.2%). Age, diabetes, hypertension, atypical chest pain, and ACS were HEART score predictors. The mean HEART scores of hospitalised and discharged patients were 3.3 ± 1.60 and 1.4 ± 1.19, respectively. The concordance between ED and HEART score disposition was 43.4% for home discharged; and 91.0% for hospitalised patients. The percentage of patients discharged home after ED diagnosis was significantly lower than the percentage that would have been discharged based on the HEART score assessment (p ≤ 0.001).
Conclusion: The disposition plan for patients presenting with chest pain based on ED diagnosis errs on the side of caution. Compared to clinical decision-making using the HEART score, it is somewhat conservative.
Background
Chest pain as a presenting symptom is common in the emergency department (ED) and accounts for 5% to 6% of ED patients in the United States [1,2]. Chest pain can result from a wide range of aetiologies from benign conditions such as muscular pain, atypical chest pain, anxiety, and stress to life-threatening conditions like acute pericarditis, aortic dissection, pulmonary embolism, and cardiac ischaemia [3]. Distinguishing between these causes is of utmost importance to allow for safe and effective management. Life-threatening conditions require prompt diagnosis and early treatment to prevent complications [4], increasing the patient's chances of survival [5]. For benign conditions, being overly cautious may result in avoidable admissions at a tremendous cost without any significant value to the patient or the health care system [6]. The majority (58.7%) of chest pain presentations are non-cardiac in origin and are classified as 'anxiety', 'panic', or 'chest pain of unknown cause' [7]. Patients with these conditions may be discharged home. To optimise outcomes and minimise costs, numerous clinical decision-making instruments have been researched for screening and treating chest pain in the ED. These tools can minimise the risk of incorrect or inappropriate diagnosis, delayed treatment, or even loss of life. In addition, the accompanying emotional and social problems associated with these risks can be reduced [8] along with the legal and economic consequences [9].
Screening tools such as the Thrombolysis in Myocardial Infarction (TIMI) risk score [10] and the History, Electrocardiogram (ECG), Age, Risk factors, and Tropon in level (HEART) score [11] are used to assess the severity of chest pain [12] and improve case management [4]. The HEART score helps to stratify patients into low, intermediate, or high-risk categories and is designed to assess patients suspected of cardiac chest pain during the emergency. Scores such as the TIMI stratify the risk for heart events in patients with high-risk for or currently active acute coronary syndrome (ACS) to decide intervention strategies (surgical or otherwise). The aim of this study was to evaluate and compare the actual patient discharge dispositions (admission or discharge) from the ED of a tertiary health care institute in a resource-limited country with retrospectively determined disposition recommendations based on the HEART score.
Patients and Methods
The target population in this retrospective study included all patients with chest pain who reported to the ED of the largest public tertiary health care institute in Trinidad, the San Fernando General Hospital, which serves about 600,000 patients [13]. The hospital provides free, convenient, 24-hour service and is open to everyone, resulting in most island residents and visitors seeking medical care at this institution. Some patients, however, choose to attend private health institutions for treatment.
The sample comprised of patients presenting to the ED with chest pain from 2 May 2015 to 26 August 2015 (117 days). There was no reason to believe that patients admitted prior to 2 May differed significantly from those included in the study sample. Patients with chest pain were identified between 8 and 9 am each day except on weekends and public holidays. Weekend and public holiday patients' records were reviewed on the following day. Patient names were cross-referenced with those on a computerised medical records system (Selma, CNS a.s., Czech Republic), and the patient medical record cards from the ED filing room. The sample consisted of patients who were at least 18 years old with useable records, as well as a diagnosis of documented chest pain as assessed by the ED physician. Prior to data collection, all participating staff members, including nurses, doctors, and clerks were trained according to the study protocol.
Data were collected from the medical record cards using a pilot-tested questionnaire. The pilot allowed for changes, thereby preventing ambiguity in or irrelevance of the questions. The relevant questions included sections on the patient socio-demographics (age, sex, ethnicity, marital status), presenting symptoms, medical history, results of laboratory and radiographic investigations (blood counts, ECG, chest X-ray, computed tomography [CT], and echocardiography), ED diagnosis, treatment, discharge, and referrals. Some patients were assessed as having atypical chest pain. Atypical chest pain is defined as chest pain not classical of angina but presenting as chest burning, sharp, and can also occur from a number of non-cardiac factors.
Of the two categories of ED patients (admitted or discharged), discharged patients can be DAMA (discharged against medical advice) or discharged by the attending physician. Data were entered in SPSS, Version 19.0 (IBM Corp., Armonk, NY), through which further analysis was undertaken using SPSS, Version 23.0 (IBM Corp., Armonk, NY) [14].
The HEART scores were calculated by the procedure described by Six, et al. [15] for patients with chest pain in the emergency room. The HEART score is based on five factors: H (heart), E (ECG), A (age), R (risk factors), and T (trop on in levels). Each factor was scored 0, 1, or 2 points, depending on the severity and extent of abnormality [15]. The actual number of patients dispatched home or to a medical ward for further treatment was compared to the number that would have been dispatched using the HEART score criteria where: 0-3 points holds a low risk of 2.5% for an endpoint and supports an immediate discharge, a HEART score of 4-6 points, moderate risk of 20.3%, implies admission for clinical observation/evaluation and a HEART score ≥ 7 points, with a high risk of 72.7%, supports early invasive strategies [11].Cohen's kappa was used to compare the level of agreement between the ED disposition and disposition determined using the HEART score in retrospect. See (Table 1) for interpretation of kappa scores.
Prior to the use of Analysis of variance (ANOVA), HEART scores were computed as proportions (out of 10) and the Arcsine transformation was used to convert the corresponding data in order to satisfy one of three necessary and sufficient requirements for using this ANOVA to compare means; namely, that they have a Normal distribution with finite mean and finite variance . Heart scores are integers and hence are not continuous; and do not have a Normal distribution; hence they could not be used for ANOVA. There was no reason to believe that the other two conditions; namely, that the HEART score were independent and identically distributed were both satisfied.
Data are described with frequency and percentage distribution tables, graphs, and selected summary statistics. The inferential methods included chi-square hypothesis testing and analysis of variance (ANOVA) with 95% confidence intervals (CIs).
The collected data was kept confidential, and only the researchers, statistician, and research assistants were granted access. The Clinical Governance and Ethics Committee of the South-West Regional Health Authority granted ethical approval on 28 April 2015, operating from San Fernando, Trinidad and Tobago. Since the data from the medical records was de-identified, the ethics committee did not require informed consent from each patient.
Results
Socio-demographics
During the study period (2 May 2015 to 26 August 2015 [117 days]), a total of 11,941 patients visited the ED. Of these, the records of 1014 (8.5%) patients who presented with chest pain were reviewed. Of these, 29 were excluded: Sixteen (1.6%) were under 18 years of age and thirteen (1.3%) had inadequate or unsatisfactory data (Figure 1).
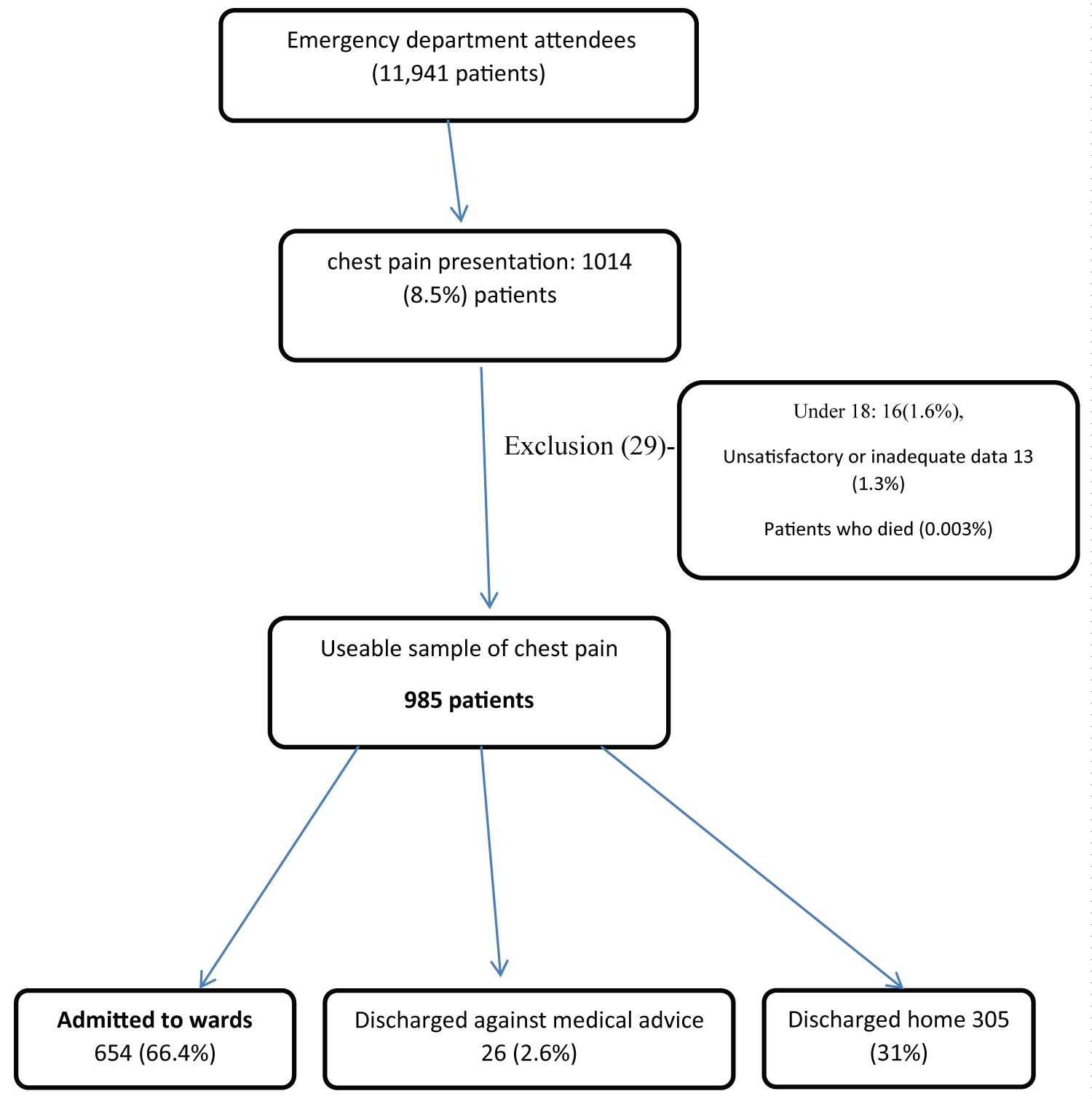
Figure 1: Emergency department patients with chest pain.
A total of 985 records were useable and formed the basis of all the findings reported hereafter. The majority of patients were female (n = 512; 52.7%), ≥ 65 years of age (n = 265; 26.9%), and of Indo-Trinbagonian descent (n = 580; 58.9%) (Table 2).
Table 2: Distribution of selected demographic variables. View Table 2
Additional presenting symptoms in the sample group ranged from atypical chest pain (0.9%) to shortness of breath (n = 450, 45.4%) (Table 3). Symptoms showing a frequency of < 1% included anxiety, near fainting, and fatigue.
Table 3: Additional presenting symptoms in the sample group. View Table 3
Emergency department diagnosis/dispatch/cardiovascular risk distribution
In the ED, following initial triage of chest pain, patients were reviewed by the emergency physician with the supervision of a registrar. The diagnosis was made by the attending physician or in unclear cases by a senior doctor. The diagnosis was made based mainly on medical history, physical examination, and relevant investigations such as ECG and troponin blood tests within the initial presentation to the ED. More than half (n = 577, 58.6%) of the patients did not have ACS, 5.7% (n = 56) were diagnosed with acute myocardial infarction (AMI), and 2.0% (n = 20) had ST-segment elevation myocardial infarction (Figure 2). Chi-square analysis showed that ED diagnoses were independent of sex, age group, and ethnicity.
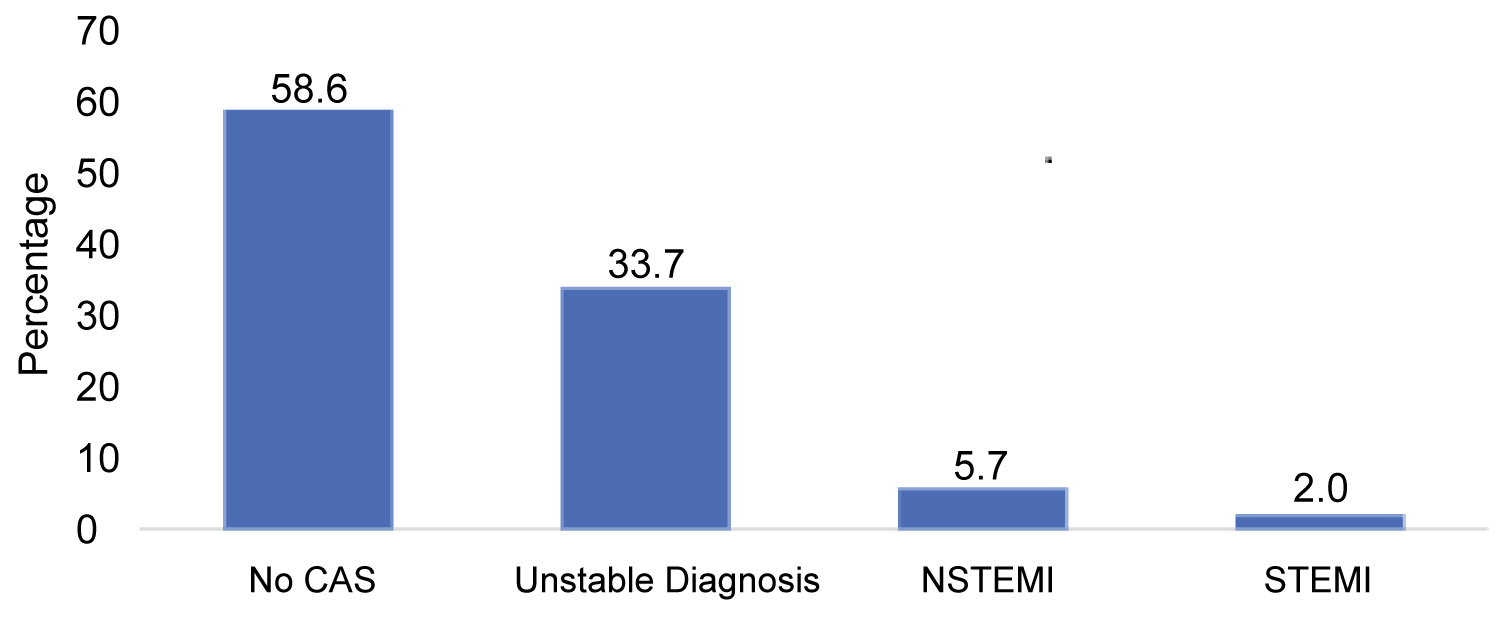
Figure 2: Emergency department (ED) diagnosis (N = 985).
Abbreviations: ACS: Acute Coronary Syndrome; ER: Emergency Room; STEMI: ST-Segment Elevation Myocardial Infarction; NSTEMI: Non-ST-Segment Elevation Myocardial Infarction
Of the patients presenting with chest pain, 2.6% were DAMA and 31% were discharged home (Figure 3). Admission to non-medical wards was due to inadequate bed availability in the medical wards. Patients who were hospitalised (66.4%) were older than those who were discharged by physician and those who were DAMA. The mean ages of patients who were DAMA, those discharged home, and those who were hospitalised were 50.0 (± 16.73) years, 41.6 (± 15.38) years, and 58.4 (± 14.5) years, respectively. In addition, with respect to disposition, disposition (admission, or discharge) were associated with sex (chi-square = 4.084, degrees of freedom [df] = 1, p = 0.025), age (chi-square = 219.497, df = 5, p = ≤ 0.001), and ethnicity (chi-square = 35.768, df = 52, p = ≤ 0.001). Specifically, the percentage of males warded (71.7%) was significantly higher than the percentage of females (65.5%). A significantly larger proportion of Indo-Trinbagonians (75.1%) than Afro-Trinbagonians (56.2%) or patients of mixed ethnicity (55.2%) were hospitalised. Finally, the probability of being hospitalised increased with age among patients ≥ 40 years (Figure 4).
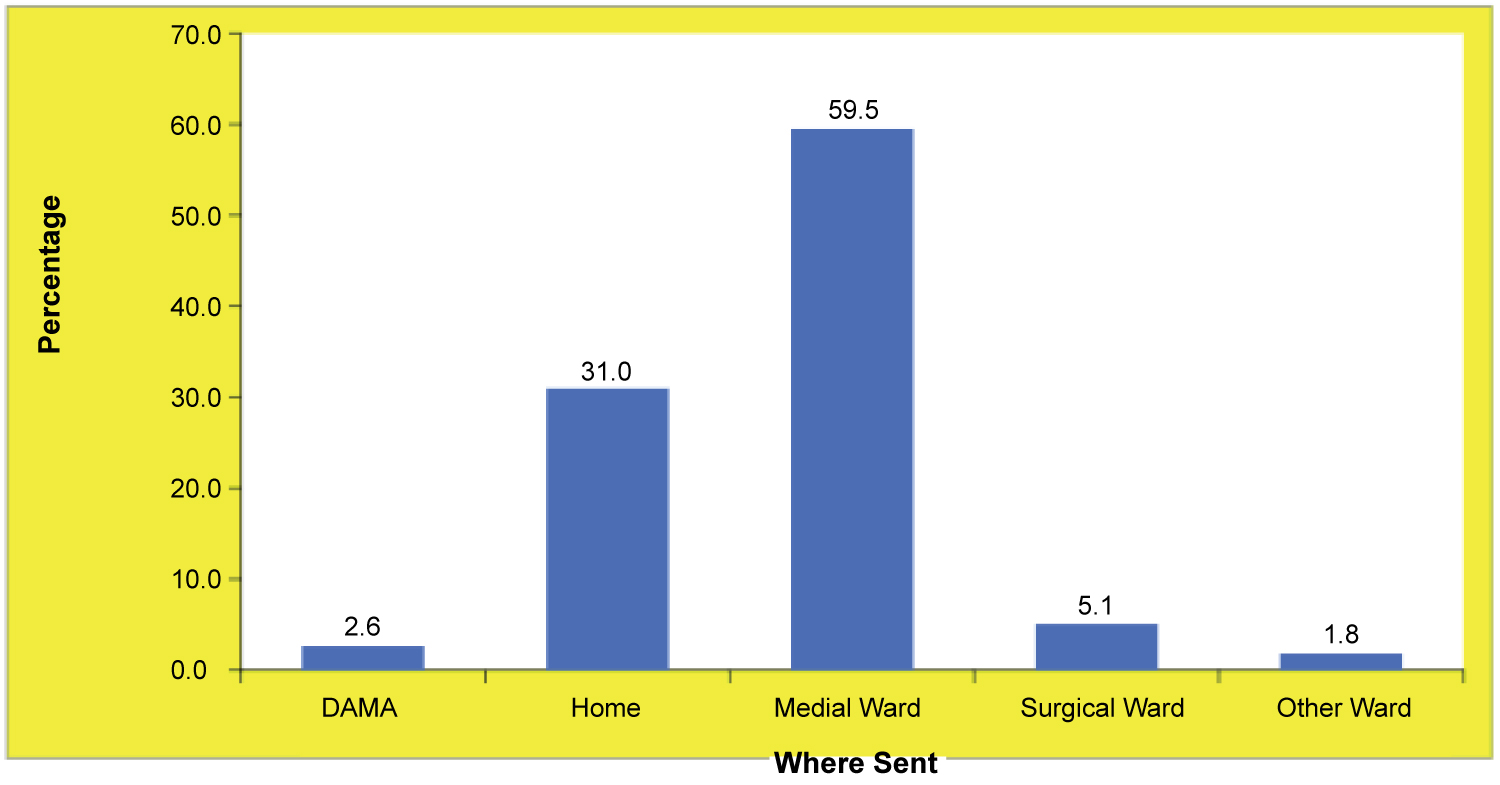
Figure 3: Patient discharge after ED diagnosis.
DAMA: Discharged against Medical Advice.
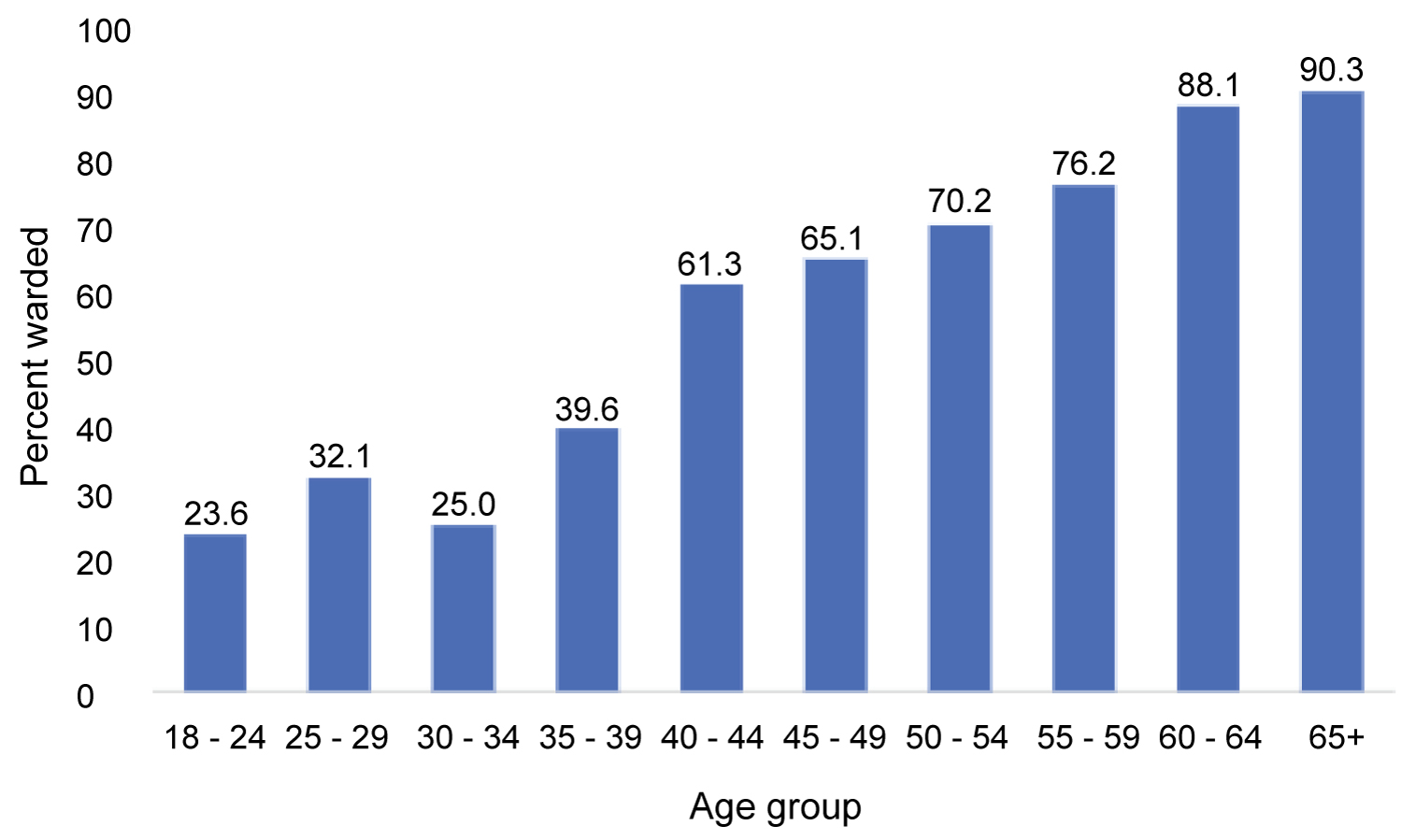
Figure 4: Percentage of patients hospitalised according to age group.
The characteristics of the patients were different for each type of disposition. Hospitalised patients were distributed equally between males and females but were predominantly Indo-Trinbagonians (65.6%) and over 50 years of age (75.8%). The hospitalised patients showed no significant difference between the mean age of male and female patients (p = 0.607) or among the three ethnic groups (p = 0.080). Of the 305 patients who were discharged by physician after diagnosis in the ED, the majority were female (n = 175; 57.4%) and predominantly Indo-Trinbagonian (n = 142; 46.6%). However, there was no difference between the mean age of male and female patients (p = 0.769) or among the three ethnic groups (p = 0.949).
More than half the patients who were DAMA (14/26, 53.8%; 95% CI [33.4, 73.4]) had 1 to 3 risk factors, 51.7% (95% CI [50.9, 62.4]) of the patients discharged by physicians had no risk factors, and 72.9% (95% CI [68.9, 75.9]) of the hospitalized patients had 1 to 3 risk factors (Table 4). Overall, only 2.8% (27/985, 95% CI [1.8, 4.0]) of patients had more than three risk factors (such as diabetes mellitus, hypertension, hyperlipidaemia, smoking, sedentary lifestyle, family history of ischemic heart disease (IHD), apolipo protein (apo)-A/apo-B, stress/depression (Table 4).
Table 4: Distribution of the number of HEART SCORE risk factors according to emergency room disposition. View Table 4
Overall, the majority of patients presenting with chest pain had hypertension (44.5%) or diabetes mellitus (33.3%) (Table 5). However, the prevalence of cardiovascular (CV) risk in each category was markedly different. Among the hospitalised patients, the proportion of patients with hypertension and diabetes mellitus accounted for 83.1% and 84.1% of the total, respectively, while in patients discharged to home, these CV risks accounted for just over 10% of patients with chest pain (Table 5). Diabetes, hypertension, IHD, and a history of previous heart attack (p ≤ 0.001) were the only associated risk factors with ED patient disposition. Specifically, patients with at least one of these CV risks were more likely to be hospitalised after diagnosis in the ED than patients with other health conditions (Table 5). A comparison of the relative risk (RR) of being hospitalised or not with 95% CI is shown in Table 6 for selected variables. A history of heart attack, IHD, hypertension, or diabetes mellitus carried the highest RR of being hospitalised (Table 6).
Table 5: Selected patients' medical and lifestyle history according to emergency room disposition. View Table 5
Table 6: Relative risk (RR) of being hospitalised after emergency department diagnosis as per the selected health condition. View Table 6
HEART score status and associated factors
The minimum HEART score was 0 (n = 114; 11.6%), maximum was 8 (n = 2; 0.2%), modal and median scores were both 3 (n = 199; 20.2%), and mean was 2.70 (± 1.721). Patients who were hospitalised had higher mean scores than patients who were discharged home and DAMA. (Table 7) shows the mean (± standard deviation [SD]) and the corresponding 95% CIs for the HEART scores according to ED disposition. The ANOVA showed that ethnicity (p = 0.235) and history of a previous heart attack (p = 0.168) were not significantly associated with the mean HEART score (Table 8).
Table 7: HEART score descriptive and inferential statistics by emergency room (ER) disposition. View Table 7
Table 8: Analysis of Variance (ANOVA): Transformed HEART score. View Table 8
Multivariable linear regression
A plot of the mean HEART score versus age showed that a quadratic function may be a good fit for the functional relationship between these two variables (Figure 5). It was clear, however, that the true functional relationship was better represented by a multivariable relationship, preferably linear, for easy interpretation.
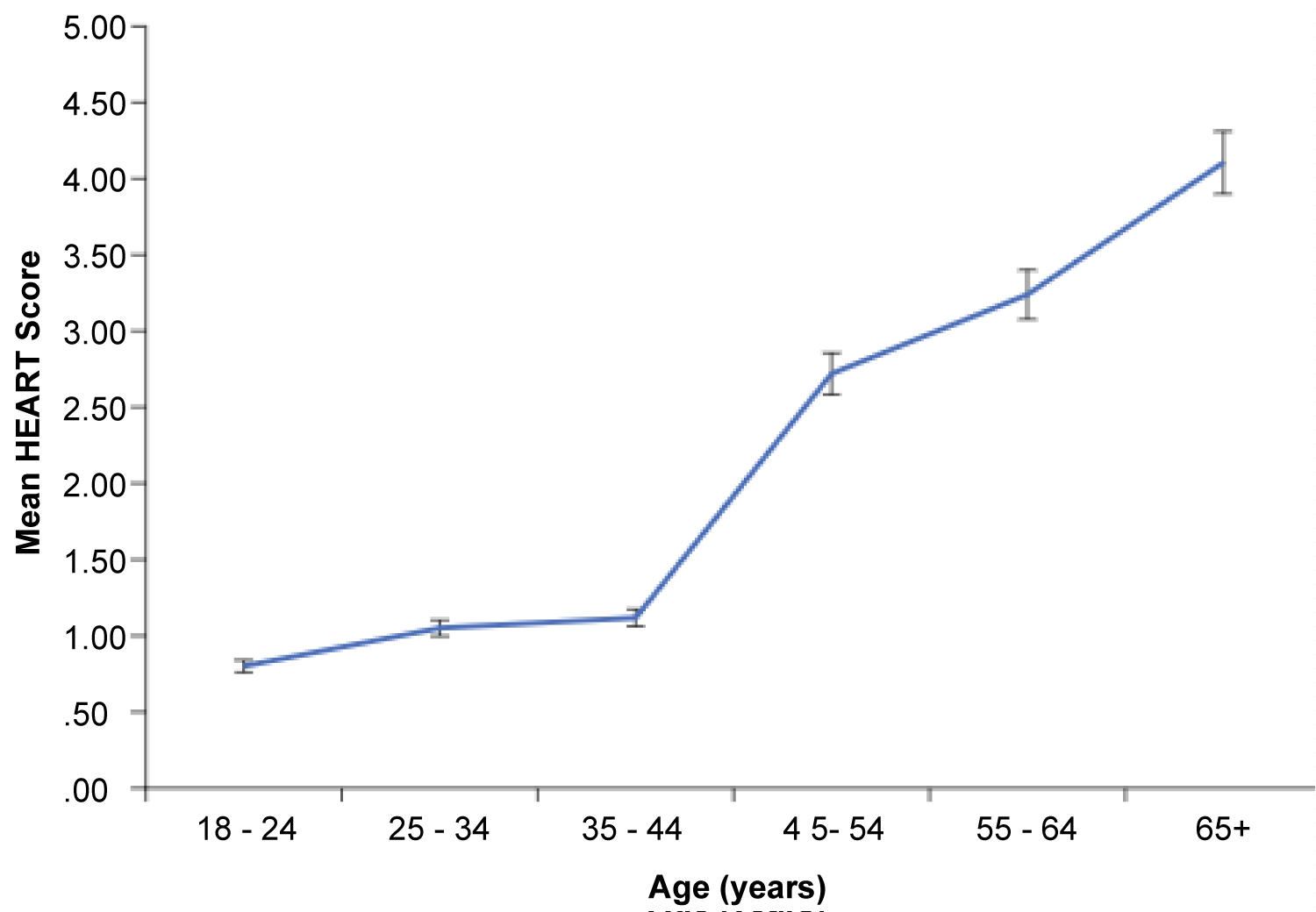
Figure 5: Mean HEART score based on patients' ages.
Subsequent multivariable linear regression analysis showed that age (p ≤ 0.001), sex (p = 0.007), diabetes (p ≤ 0.001), hypertension (p ≤ 0.001), IHD (p ≤ 0.001), atypical chest pain (p = 0.035), and the ACS type (p ≤ 0.001) were predictors of the HEART score (Table 9). The lack of fit did not appear to be substantial (R2 = 0.620, adjusted R2 = 0.618).
Table 9: Table of regression coefficients. View Table 9
Emergency department disposition and HEART score disposition: Cohen's kappa
The concordance and discordance between ED disposition and HEART score disposition are shown in Table 10. Both methods showed agreement with respect to the disposition of 586 (61.1%) patients, divided between those discharged home (n = 285) and those admitted or warded (n = 301). The discordance was high regarding the number of patients admitted based on the ED diagnosis but who qualified for discharge home according to the HEART score criteria. A total of 353 (36.8%) of the 959 patients were in this category.
Table 10: Emergency Department (ED) disposition vs. HEART Score disposition. View Table 10
Cohen's kappa was used to measure the reliability using the HEART score method as the gold standard (Table 11). The null hypothesis of no agreement between ED disposition and HEART score disposition was rejected (p ≤ 0.001). However, the kappa measure of agreement (0.306, 95% CI [0.281, 0.349]) was fair at best using the Landis & Koch [14] interpretation.
Table 11: Measure of agreement (Cohen's kappa). View Table 11
Of the 26 patients DAMA, 6 (30.8%) satisfied the HEART score criteria for being admitted.
Discussion
General (diagnosis, prevalence, and dispatch)
This study found that the disposition of patients presenting with chest pain based on ED diagnosis erred on the side of caution; thus, the agreement with HEART score disposition was 'fair'. At the study site, patients with chest pain accounted for 8.5% of emergency admissions. This is similar to the findings of the chest pain evaluation registry (CHEPER) study (5.3%) [2], as well as 6% found in England and Wales [17] and 5%in the USA [18]. Among the hospitalised patients, suspected ACS accounted for 41.4% of the patients. This is similar to other studies that reported 11% to 39% of coronary artery disease (CAD) patients experienced chest pain [19], 45% to 50% of ED patients have cardiac-related chest pain [20], and 50% to 55% of patients experience non-cardiac chest pain [21,22].
In terms of ED disposition, our study revealed that 31% of the patients were discharged home and 66.4% were admitted; the rest were DAMA. These results were independent of age, sex, and ethnicity. According to Eichel Berger, et al. over 80% of CAD patients were admitted [23]. Koukkunen, et al. reported 25% (n = 764) of patients were discharged home, 417 or 13% were discharged after observation, and 1702 patients were hospitalised [24].
In our study, 41.4% of patients presenting with chest pain to the ED were diagnosed with ACS; 81.4% of ACS patients had unstable angina while 12.9% had non-ST-segment elevation myocardial infarction (NSTEMI). This is similar to the findings of Belguith, et al. who reported that 49.7% of non-traumatic chest pain cases were due to ACS, and 74.2% of ACS cases comprised unstable angina/NSTEMI [25].
Characteristics of patients: Hospitalised versus discharged
In our study, the majority (72.9%) of hospitalised patients had 1 to 3 cardiovascular risks, (predominantly diabetes mellitus, hypertension, previous myocardial infarction, IHD, smoking, and hyper cholesterolaemia). In contrast, the majority of discharged patients had no risk factors. Risk factors were more prevalent in premature ACS patients compared with the general population especially among young women with a family history of CAD [26]. The hospitalised patients were generally older (mean 58.4 [± 14.5] years), distributed equally among males and females, and > 50 years of age (75.8%) compared to those who were discharged. There was no significant difference between the mean age of male and female patients (p = 0.607) or among the three ethnic groups (p = 0.080). These findings contrast with those of a study conducted in the United States by Trivedi, et al., which revealed that acute myocardial infarction is more likely to be common among young black women [27].
The absence of any CV risk in the majority (51.7%) of discharged patients was similarly observed in a study by Lau, et al. who found that patients discharged from EDs were less likely to have diabetes, hypertension, or prior heart diseases [28]. Our study also revealed that of the 407 patients clinically assessed as having ACS, 19 (4.7% of ACS cases) were discharged home. These patients may be at low risk for future heart events, with doctors willing to discharge such patients.
HEART score
In our study, the mean HEART score of the hospitalised patients was 3.3 ± 1.60 compared to that of patients discharged home (1.4 ± 1.19). A comparison of potential disposition based on the HEART score and current practices revealed a high percentage of concordance with 91% agreement on the decision to admit patients. However, there was only 43.4% agreement on who should be discharged home. Based on the HEART score, more patients would be eligible for discharge home. Out of the 654 actual admissions, the expected number of admissions based on the HEART score should have been 329 patient admissions. Similar findings were reported where more than twice the number of patients were hospitalised than there would have been, had the admissions been based on the HEART scores [15,29]. The relatively low mean HEART score of the hospitalised patients and the discordant pairs could be attributed to the habit of erring on the side of caution in medical diagnosis. However, low-risk patients can usually be managed at chest pain units using serial ECGs and cardiac injury markers [30]. Furthermore, low-risk patients can be sent home within 24 hours and can undergo tests for ischaemia at a later date or have tests for myocardial ischaemia done on the same day [31]. A high admission rate may be due to other reasons for admission, ignorance, fear of litigation, or unclear guidelines for admission and discharge. The utilisation of the HEART score may decrease unnecessary admissions and avoid needless discharge. A study by Smulowitz, et al., when implementing the HEART score, led to a small (8.4%) but significant decrease in admissions [32]. Kuhlman, in his analysis of the HEART score, emphasised its use coupled with a supportive outpatient infrastructure to facilitate the safe disposition of undifferentiated chest pain presenting to the ED [33]. The HEART score, with its five parameters based on ED patients with chest pain, is preferred because of its appropriateness in this setting, ease of use [34], "ready availability of the variables under consideration, and focus on short-term outcomes" [11]. The HEART score also provides reassurance that for low-risk patients, early discharge is safe [35]. It is also "designed to be faster, simpler, and more intuitive" than the other ACS risk-scoring systems such as the TIMI or GRACE [36], a modified HEART score that has also been used in clinical settings [37].
Limitations
This was a single-centre study with data collected over a short period. This selection bias makes the result not generalizable. The retrieval of patient records on days following public holidays was challenging; consequently, not all records could be retrieved. Presentation of chest pain, though the most common presentation of IHD, does not include all patients with IHD or ACS because many cases of myocardial ischaemia present differently. As reported by Coven, patients can present with no pain, episodic shortness of breath, severe weakness, light-headedness, diaphoresis, or nausea and vomiting [38]. In a busy hospital and the absence of a working chest pain protocol, pertinent information may be missing. The HEART score is subject to variations in the physicians' perception of significant history/physician experience. Finally, there was no follow-up of patient outcomes.
Conclusion/Recommendations
In this study, we found that disposition practices practiced by physicians compared to the HEART score erred on the side of caution by admitting more patients. Countries with limited resources should take advantage of the HEART score to improve patient disposition from the ED. The HEART score identifies a substantial number of low-risk patients. For low-risk patients, the CV risk must be weighed against the inconvenience of tests/hospitalisation and the additional substantial expenditure, which is particularly challenging in resource-limited countries. In addition, patients warranting urgent surgical intervention can be identified and managed appropriately. HEART score screening, owing to its objectivity, should be encouraged in the ED, coupled with proper training and appropriate diagnostic tools. Future research is required to evaluate patients' disposition particularly those discharged home.
Declarations
Ethics approval and consent to participate
This study was granted ethics approval by the Ethics Committee of the South-West Regional Health Authority and the University of the West Indies. Informed consent was waived.
Consent for publication
Not applicable.
Availability of data and material
The data that support the findings of this study are available from the corresponding author on request.
Competing interests
The authors declare that they have no competing interests.
Funding
Not applicable.
Acknowledgements
We would like to thank the pre-medical students who assisted in data collection.
References
- Zalenski RJ, Rydman RJ, McCarren M, et al. (1997) Feasibility of a rapid diagnostic protocol for an emergency department chest pain unit. Ann Emerg Med 29: 99-108.
- Graff LG, Dallara J, Ross MA, et al. (1997) Impact on the care of the emergency department chest pain patient from the chest pain evaluation registry (CHEPER) study. Am J Cardiol 80: 563-568.
- Kontos MC, Diercks DB, Kirk JD (2010) Emergency department and office-based evaluation of patients with chest pain. Mayo Clin Proc 85: 284-299.
- Hamm CW, Goldmann BU, Heeschen C, et al. (1997) Emergency room triage of patients with acute chest pain by means of rapid testing for cardiac troponin T or troponin I. N Engl J Med 337: 1648-1653.
- Beck AJ, Hagemeijer A, Tortolani B, et al. (2015) Comparing an unstructured risk stratification to published guidelines in acute coronary syndromes. West J Emerg Med 16: 683-689.
- Groarke J, O’Brien J, Go G, et al. (2013) Cost burden of non-specific chest pain admissions. Ir J Med Sci 182: 57-61.
- McDevitt-Petrovic O, Kirby K, Shevlin M (2017) The prevalence of non-cardiac chest pain (NCCP) using emergency department (ED) data: a Northern Ireland based study. BMC Health Serv Res 17: 549.
- Polsky D, Doshi JA, Marcus S, et al. (2005) Long-term risk for depressive symptoms after a medical diagnosis. Arch Intern Med 165: 1260-1266.
- Pope JH, Aufderheide TP, Ruthazer R, et al. (2000) Missed diagnoses of acute cardiac ischemia in the emergency department. N Engl J Med 342: 1163-1170.
- Rao SS, Agasthi P (2020) Thrombolysis in Myocardial Infarction (TIMI) risk score. Stat Pearls.
- Brady W, de Souza K (2018) The HEART score: a guide to its application in the emergency department. Turk J Emerg Med 18: 47-51.
- Markel D, Jeremy Kim (2017) Identifying emergency department patients with chest pain who are at low risk for acute coronary syndromes. Emerg Med Pract 19: 1-24.
- http://www.swrha.co.tt/content/about-swrha
- IBM Corp (2015) IBM SPSS Statistics for Windows, Version 23.0. Armonk, NY: IBM Corp.
- Six AJ, Backus BE, Kelder JC (2008) Chest pain in the emergency room: value of the HEART score. Neth Heart J 16: 191-196.
- Landis JR, Koch GG (1997) The measurement of observer agreement for categorical data. Biometrics 33: 159-174.
- Goodacre S, Cross E, Arnold J, et al. (2005) The health care burden of acute chest pain. Heart 91: 229-230.
- Curfman G (2018) Acute chest pain in the emergency department. JAMA Intern Med 178: 220.
- Kachintorn U (2005) How do we define non-cardiac chest pain? J Gastroenterol Hepatol 20: S2-S5.
- Sheps DS, Creed F, Clouse RE (2004) Chest pain in patients with cardiac and noncardiac disease. Psychosom Med 66: 861-867.
- Eslick GD, Jones MP, Talley NJ (2003) Non-cardiac chest pain: Prevalence, risk factors, impact and consulting-a population-based study. Aliment Pharmacol Ther 17: 1115-1124.
- Pollack CV, Perman SM (2017) Chest pain in the emergency department: differential diagnosis. Der Internist 58: 3-7.
- Eichelberger C, Patel A, Ding Z, et al. (2020) Emergency department visits and subsequent hospital admission trends for patients with chest pain and a history of coronary artery disease. Cardiol Ther 9: 153-165.
- Koukkunen H, Pyörälä K, Halinen MO (2004) Low-risk patients with chest pain and without evidence of myocardial infarction may be safely discharged from emergency department. Eur Heart J 25: 329-334.
- Belguith AS, Beltaief K, Msolli MA, et al. (2018) Management of acute coronary syndrome in emergency departments: A cross sectional multicenter study (Tunisia). BMC Emerg Med 18: 50.
- Choi J, Daskalopoulou SS, Thanassoulis G, et al. (2014) Sex- and gender-related risk factor burden in patients with premature acute coronary syndrome. Canadian J Cardiol 30: 109-117.
- Trivedi AN, Nsa W, Hausmann LRM, et al. (2014) Quality and equity of care in U.S. hospitals. N Engl J Med 371: 2298-2308.
- Lau G, Koh M, Kavsak PA, et al. (2020) Clinical outcomes for chest pain patients discharged home from emergency departments using high-sensitivity versus conventional cardiac troponin assays. Am Heart J 221: 84-94.
- Backus BE, Six AJ, Kelder JC, et al. (2010) Chest pain in the emergency room: A multicenter validation of the HEART score. Crit Pathw Cardiol 9: 164-169.
- Amsterdam EA, Kirk JD, Bluemke DA, et al. (2010) Testing of low-risk patients presenting to the emergency department with chest pain: A scientific statement from the American Heart Association. Circulation 122: 1756-1776.
- Arnett DK, Blumenthal RS, Albert MA, et al. (2019) 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: A report of the American College of Cardiology/American Heart Association Task Force on clinical practice guidelines. J Am Coll Cardiol 74: e177-e232.
- Smulowitz PB, Dizitzer Y, Tadiri S, et al. (2018) Impact of implementation of the HEART pathway using an electronic clinical decision support tool in a community hospital setting. Am J Emerg Med 36: 408-413.
- Kuhlman J, Moorhead D, Kerpchar J, et al. (2019) Clinical transformation through change management case study: chest pain in the emergency department. E Clinical Medicine 10: 78-83.
- Backus BE, Six AJ, Kelder JH, et al. (2011) Risk scores for patients with chest pain: Evaluation in the emergency department. Curr Cardiol Rev 7: 2-8.
- Gomez R (2018) HEART score for predicting adverse outcomes in patients with chest pain. Am Fam Physician 98: 72-75.
- Jancin B (2009) HEART score predicts chest pain outcomes. Cardiology News.
- McCord J, Cabrera R, Lindahl B, et al. (2017) Prognostic utility of a modified HEART score in chest pain patients in the emergency department. Circ Cardiovasc Qual Outcomes 10: e003101.
- Coven DL (2020) Acute coronary syndrome clinical presentation.
INDEXING
PARTNERS









Table 1: Interpretation of kappa (Landis & Koch, 1977) [16]. View Table 1