-
Address:
17888 67th Court North
Loxahatchee, FL
-
Mail us:
contact@wrightacademia.org
- submit manuscript
Table of content
Research Article |
Open Access |
Volume 1 | Issue 1 |
Technique and Interpretation of Foetal Echocardiograms
Jasvinder Kaur
Paediatric Cardiologist, National University of Malaysia Medical Centre, Malaysia
*Corresponding author: Dr. Jasvinder Kaur, Paediatric Cardiologist, National University of Malaysia Medical Centre, Malaysia, E-mail: jasvinder_kr@yahoo.com
Citation: Kaur J (2019) Technique and Interpretation of Foetal Echocardiograms. Cardiol Cases Syst Rev. 1:005.
Copyright © Kaur J, et al.
Received: |
Accepted: |
Published: |
Foetal echocardiography is the ultrasonic evaluation of the human foetal cardiovascular system. Improved operator skill amongst physicians performing general antepartum obstetrical ultrasound, in combination with increased sensitivity of present day ultrasound systems, has resulted in improved detection of foetal cardiovascular abnormalities and increased requirements for more detailed evaluation. Congenital heart disease is the most common congenital anomaly found in the human. accurate diagnosis via foetal echocardiography allows for appropriate counseling to take place and for parents to take the opportunity to learn about the cardiac anomaly. This knowledge can allay parental fears, improve psychological state, and bolster coping skills in dealing with the birth of a child with life-threatening cardiovascular illness.
Introduction
The foetal heart is examined by a series of sequential ultrasound views, which image the cardiac connections and intracardiac structures. The connections of the foetal heart can begin to be detected abdominally by 11 weeks of gestation. However, the usual timing for complete foetal heart scanning is approximately 18-20 weeks [1]. Phased array transducers with fundamental frequencies between 4 Hz and 12 MHz are generally used. Curvilinear probes may be helpful given the wider near-field of view [2].
Indications
Indications for foetal echocardiography can be separated into maternal and fetal indications. Examples are listed in Table 1.
Examination and Technique
Success in foetal heart scanning involves skill in obtaining the optimum window, which is in turn dependent on a willingness to explore the maternal abdomen in order to approach the heart from different orientations to find the ideal, coupled with a thorough familiarity of cardiac views whatever the foetal position [1]. It should first be established that the stomach is on the left side of the foetus and on the same side as the apex. This can be readily checked by aligning the transducer in the long axis of the foetus, with the head to the right of the screen. The transducer should then be turned through 90 degree clockwise. If the foetus lies with the back down, the left of the foetus will be on the right of the screen; if the foetus lies with the back up, the left side is on the left of the screen [3]. If the transverse images demonstrate the back of the foetus on the right of the video screen, the left side of the foetus would be up (Figure 1). The transverse views of the heart are obtained by sweeping the ultrasound beam from the abdomen to the inlet of the thorax [1].
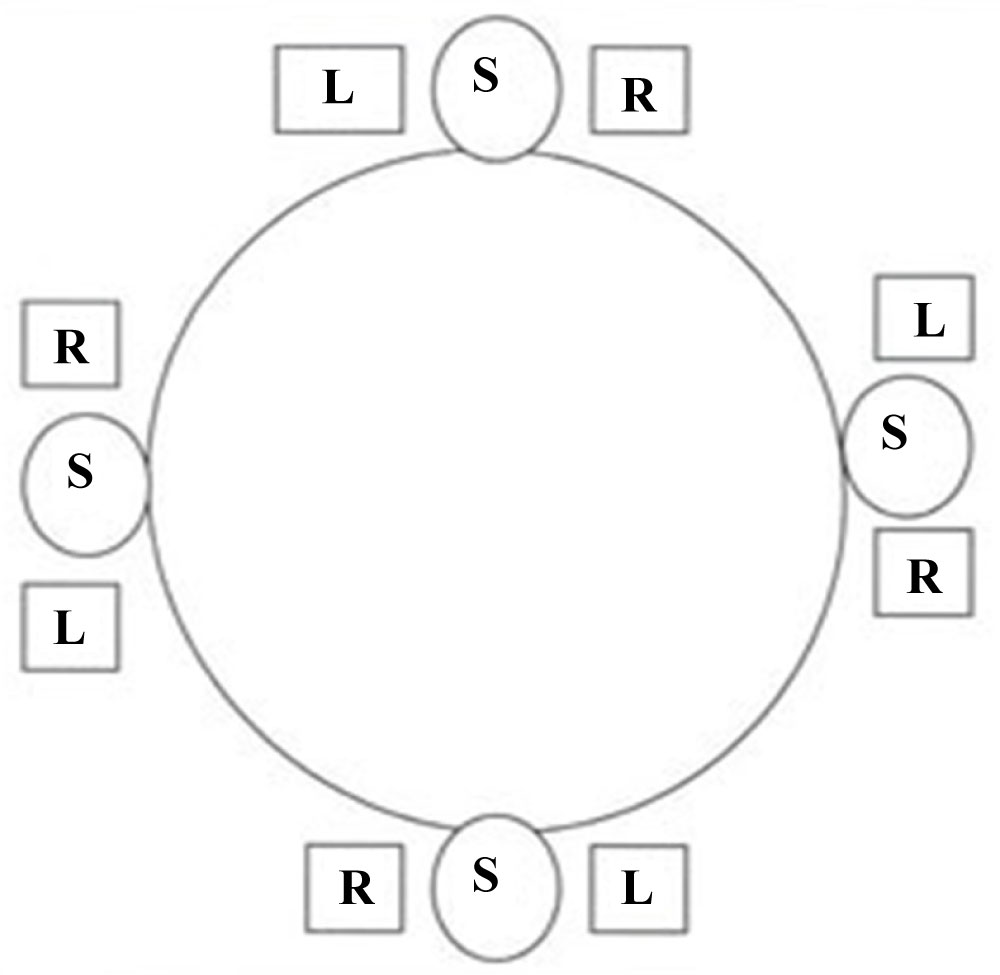
Figure 1: Schematic drawing of foetal trunk as viewed in transverse plane on video display. With foetal spine used as landmark, right and left side of foetus can be determined. Relationship of right and left side of foetus and spine are constant despite foetal rotation from face up (bottom), right side up (left), face down (top) and left side up (right). L: Left; R: Right; P: Posterior.
The standard projections that may be used in foetal heart scanning include [4] (Figure 2 and Figure 3).
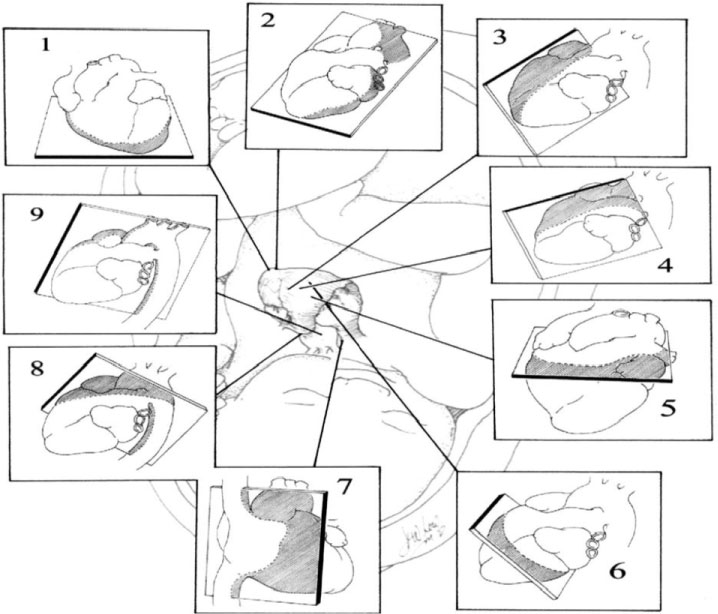
Figure 2: Illustration of the tomographic planes used to image the foetal cardiovascular system. Starting at the top left, the following views are demonstrated in a clockwise manner: 1: Apical (4-chamber) view; 2: Apical (5-chamber) view angled towards the aorta; 3: Long-axis view of the left ventricular outflow tract; 4: Long-axis view of the right ventricular outflow tract; 5: Short-axis view at the level of the great vessels; 6: Short-axis view with caudaud angling at the level of the ventricles; 7: Caval long-axis view; 8: Ductal arch view; 9: Aortic arch view.
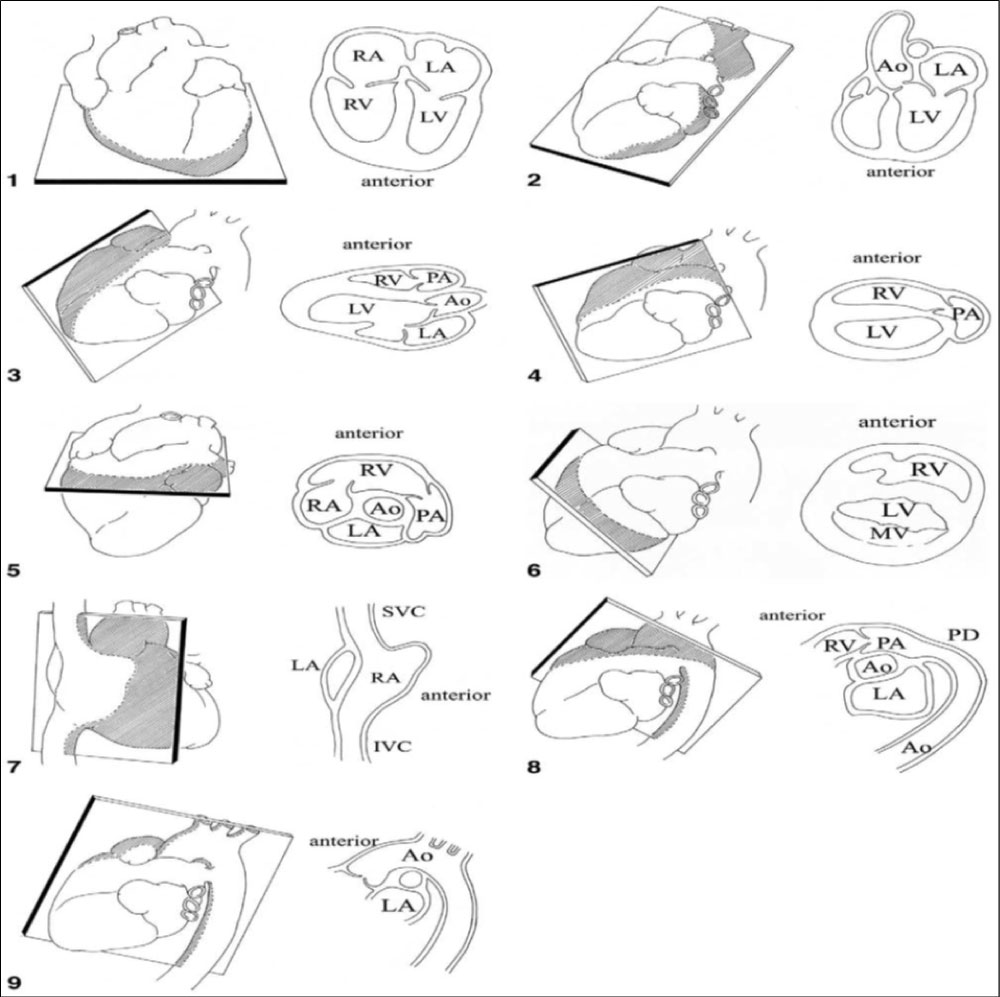
Figure 3: Illustrations of the anatomical correlates for each of the designated tomographic imaging planes used for imaging of the foetal cardiovascular system. Each numbered view relates to the clockwise illustration of the foetal heart in Figure 1. Ao: Aorta; IVC: inferior vena cava; LA: left atrium; LV: left ventricle; MV: mitral valve; PA: pulmonary artery; PD: patent ductus; RA: right atrium; RV: right ventricle; SVC: superior vena cava.
Transverse views (Table 2)
Table 2: Structures viewed in the cardiac short-axis sweep [5]. View Table 2
1. Abdomen at the level of the stomach
2. Four-cham ber view
3. Aortic origin (five-chamber view)
4. Pulmonary outflow tract (three-vessel view)
5. Transverse aortic arch.
Long-axis views
1. Short axis of the left ventricle (LV)
2. Tricuspid/aortic cut
3. Long axis of the duct
4. Long axis of the aortic arch
5. Inferior (IVC) and superior vena cava (SVC).
Angulated views
1. Long axis of the LV
2. Arch and duct simultaneously.
Transverse views of the abdomen
1. Stomac h lies on the left, in the middle of the left half of the abdomen.
2. The aorta lies anterior and to the left of the spine.
3. The IVC lies anterior to the aorta and slightly to the right of the midline.
4. The IVC and aorta are similar in size, with the aorta more pulsatile.
There should be at least five transverse images of the heart and vasculature in the view and three sagittal images:
1. Abdominal cross-sectional view (Figure 4): The stomach should be seen on the left side of the foetus and just below the heart and diaphragm. The abdominal aorta should be on the left of the spine and inferior vena cava on the right of the spine anterior to the level of the aorta [4].
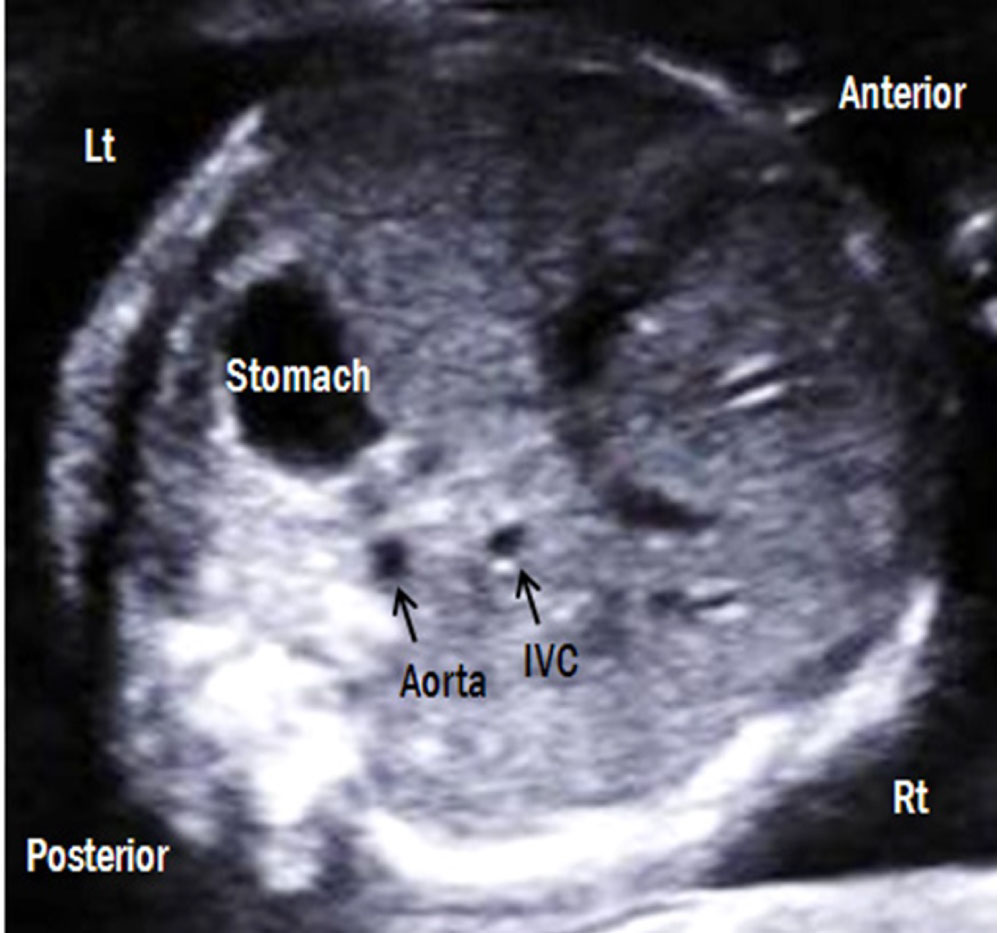
Figure 4: Transverse abdominal view. The foetal stomach is on the left side and liver is on the right side. The descending aorta is posterior-left located and the IVC is anterior-right located. Lt: left; Rt: right; IVC: inferior vena cava.
2. Transthoracic four chamber view (Figure 5): The atria should be approximately equal in size. The flap of the foramen ovale (septum primum) should move into the left atrial chamber. The ventricles should be approximately equal in size with the tricuspid valve attaching to the septum slightly apical relative to the attachment of the mitral valve. The right ventricular apex should contain the moderator band. Both ventricular chambers should reach the apex of the heart and should squeeze equally [4]. The two atrioventricular valves are equally opened and differentially inserted: The septal leaflet of the tricuspid valve is inserted more apically than the mitral valve in the ventricular septum (Table 3). Blood flow across both valves should be evaluated by colour Doppler imaging to ensure that both ventricles fill equally in diastole without regurgitation. The E wave, which corresponds to the early ventricular filing of diastole, is followed by the A wave, which corresponds to the active ventricular filling of diastole (atrial contraction). The A wave is always higher than E wave in the normal fetus. The peak velocity of both waves is 30-60 cm/sec, and is constant throughout gestation [5].
Table 3: Structures viewed in the 4- and 5- chamber view [5]. View Table 3
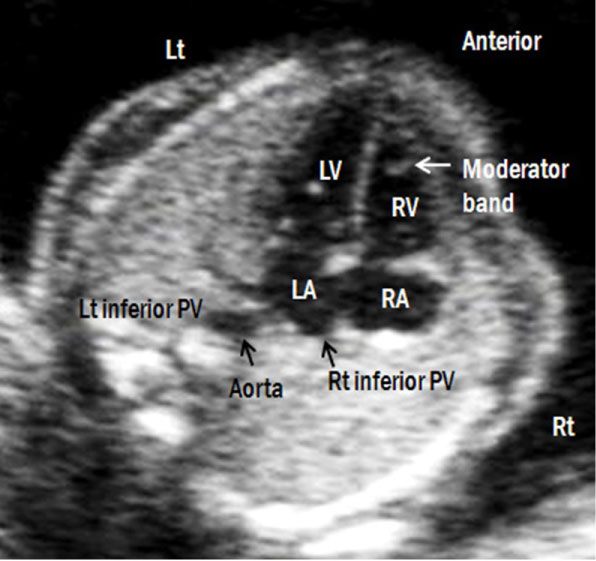
Figure 5: Apical four-chamber view of the foetal heart. Lt: left; Rt: right; LA: left atrium; RA: right atrium; LV: left ventricle; RV: right ventricle; PV: pulmonary vein.
3. Transthoracic four-chamber sweep to the Left Ventricular (LV) Outflow Tract (also known as the five chamber view) (Figure 6): Sweeping toward the foetal neck, the aortic valve and ascending aorta are seen arising centrally from the four-chamber view with the ascending aorta aiming toward the right shoulder (Table 4) [4]. Peak systolic velocity in the aorta ranges from approximately 30 cm/sec at 19 weeks to 100 cm/sec at full term [5]. Pulmonary veins should be seen in this view attached to the posterior wall of the left atrium [4].
Table 4: Structures viewed in the cardiac long-axis sweep [5]. View Table 4
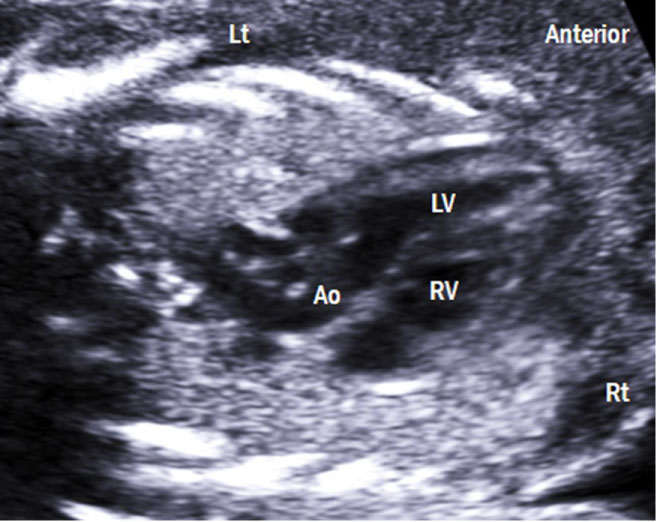
Figure 6: Left ventricular outflow tract view. (A) This view shows the ventriculoarterial connection and intact ventricular septum. Lt: left; Rt: right; LV: left ventricle; RV: right ventricle; Ao: aorta.
4. Transthoracic four-chamber sweep to the Right Ventricular (RV) Outflow Tract View: Continuing the sweep toward the foetal neck, the pulmonic valve and the main pulmonary artery are seen arising at a 90 degrees angle to the left of the ascending aorta and aiming toward the right shoulder [4]. Peak systolic velocity in the pulmonary artery increases linearly with advancing gestation, and reaches 100 cm/sec at full term [5]. The bifurcation of the pulmonary artery and ductus arteriosus completes this view [4] (Figure 7).
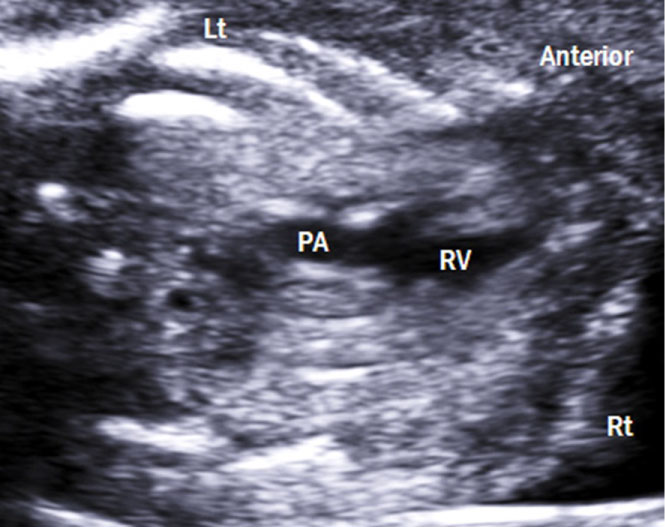
Figure 7: Right ventricular outflow tract view. This view shows the right ventriculoarterial connection. Lt: left; Rt: right; RV: right ventricle; PA: pulmonary artery.
5. The three-vessel view (Figure 8): Continuing the sweep toward the foetal neck with a medial twist of the transducer, the short axis views of the main pulmonary artery, the ascending aorta and the superior vena cava are seen with their relationships to the trachea and esophagus. The main pulmonary artery diameter is slightly greater than the aorta which is slightly greater than the superior vena cava [4].
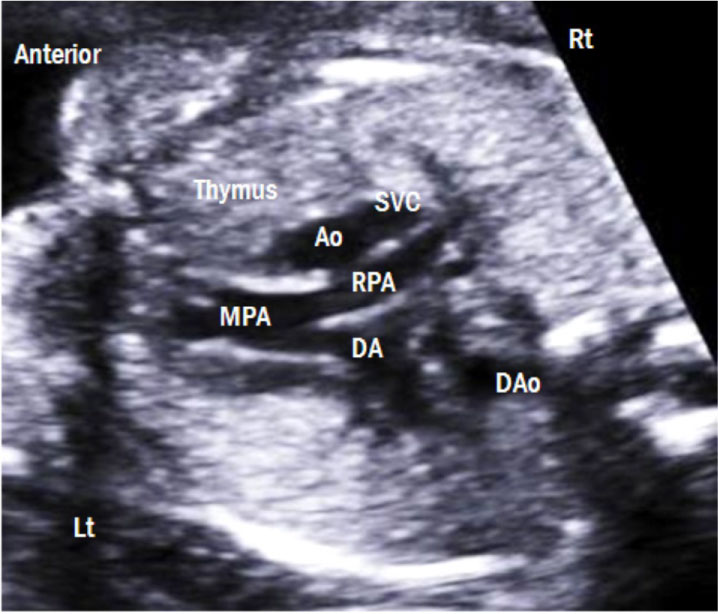
Figure 8: Three-vessel view. The main pulmonary artery, ascending aorta, and superior vena cava are arranged in a straight line from the left anterior to the right posterior aspect. The pulmonary artery is the largest in size, followed by the ascending aorta and the superior vena cava. The thymus is clearly visible anterior to the three vessels. Lt: left; Rt: right; MPA: main pulmonary artery; RPA: right pulmonary artery; DA: ductus arteriosus; Ao: aorta; SVC: superior vena cava; Dao: descending aorta.
6. Three vessel tracheal view (Figure 9): Aortic and ductal arches are combined into the DAo, which appear as a V-shaped confluence. Both arches are similar in size and located to the left side of the trachea. The thymus is also visible in this view. Colour Doppler imaging demonstrates the same direction of blood flow in both arches. This view allows comparison of both arches and assessment of aortic arch abnormalities, including aortic arch hypoplasia and coarctation of the aorta [4].
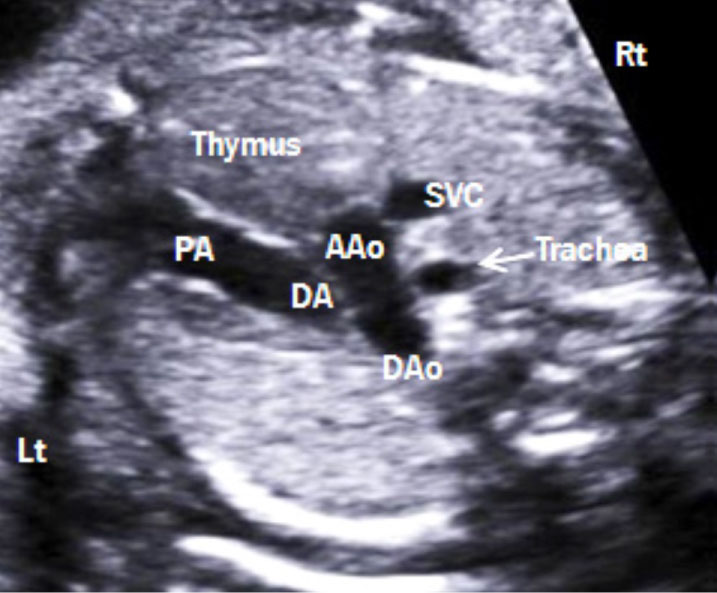
Figure 9: Three-vessel-trachea view. This view demonstrates a V-shaped confluence of aortic and ductal arches at the descending aorta. The trachea is located to the right side of the aorta. Lt: left; Rt: right; PA: pulmonary artery; DA: ductus arteriosus; Aao: ascending aorta; Dao: descending aorta; SVC: superior vena cava.
7. Aortic arch view (Figure 10): By rotating the transducer 90 degree either clockwise or counterclockwise from the 3VV, a 'candy cane-like' aortic arch is seen. The aortic arch gives rise to the three arterial branches, namely, the brachiocephalic, left common carotid, and left subclavian arteries. All three branches are clearly visible by colour Doppler imaging. Because the innominate vein is the largest vessel in the mediastinum, it is often observed in front of the brachiocephalic artery [5].
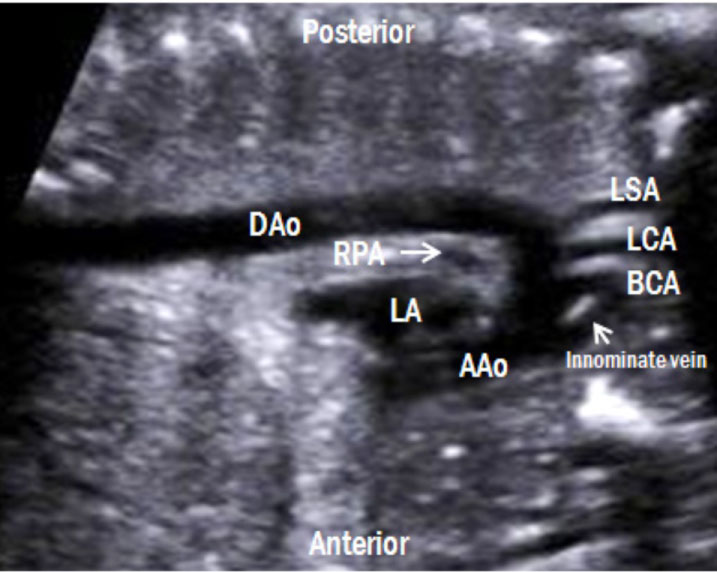
Figure 10: Aortic arch view. A 'candy cane-like' aorta gives rise to the three arterial branches, namely, the brachiocephalic, left common carotid, and left subclavian arteries. These three branches are also visible by color Doppler imaging. LA: left atrium; RPA: right pulmonary artery; Aao: ascending aorta; Dao: descending aorta; BCA: brachiocephalic artery; LCA: left common carotid artery; LSA: left subclavian artery.
8. Ductal arch view (Figure 11 and Table 5): By sliding the transducer from the aortic arch view to the left, a 'hockey stick-like' ductal arch is visualized. This view mainly shows the right ventricle, pulmonary valve, and main pulmonary artery, which is connected to the DAo through the ductus arteriosus. Unlike the aortic arch, the ductal arch does not give rise to any branches [5].
Table 5: Structures viewed in the ductal and aortic arch views [5]. View Table 5
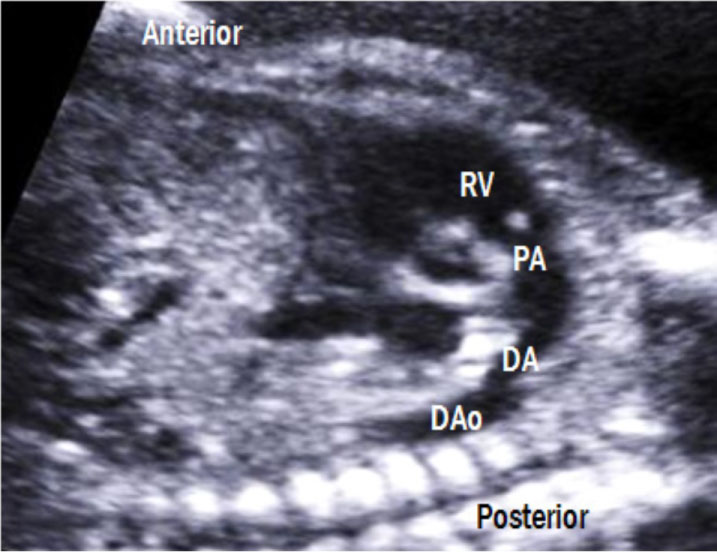
Figure 11: Ductal arch view. The ductus arteriosus connects the main pulmonary artery to the DAo, forming hockey stick-shaped arch. RV: right ventricle; PA: pulmonary artery; DA: ductus arteriosus; Dao: descending aorta.
9. Sagittal sweep view showing the superior vena cava, right atrium and inferior vena cava (Figure 12 and Table 6): Both the superior vena cava (SVC) and the inferior vena cava (IVC) drain from a posterior position to a medial connection to the right atrium. The hepatic veins descend from an anterior position to the right atrial (RA) junction with the IVC [4].
Table 6: Structures viewed in the caval long-axis view [5]. View Table 6
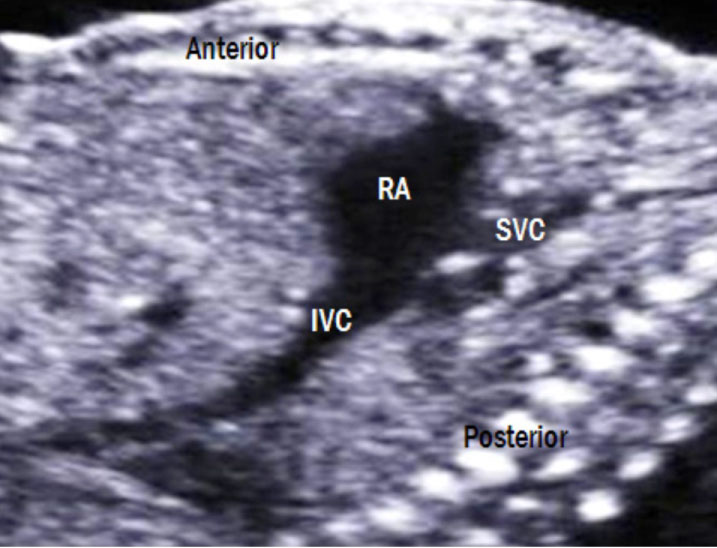
Figure 12: Bicaval view. The SVC and IVC drain into the posterior aspect of the right atrium. The IVC is widened as it enters the right atrium because of interflow from the ductus venosus and hepatic veins. RA: right atrium; IVC: inferior vena cava; SVC: superior vena cava.
10. Sagittal sweep view showing the centrally arising aortic arch: Twisting the transducer slightly to the fetal right shoulder reveals the aortic arch with the brachiocephalic vessels aiming to the foetal neck [4].
11. Sagittal sweep view showing the ductal arch: straightening out the transducer and sweeping to the left of the spine reveals the anterior, superiorly arising pulmonary artery to ductus arteriosus to descending aorta portions of the ductal arch. The branch pulmonary arteries and the ductus arteriosus are seen aiming toward the foetal abdomen [4].
Taken as a whole, these images show normalcy in the following fashion [4]:
1. Position: the axis of the foetal heart, made up of the interventricular and interatrial septa, should be seen in coming from the center of the chest into the left hemi thorax at a 45 degree angle to the sternum to spine axis in a transthoracic four-chamber view.
2. Size: in the transthoracic four-chamber view, the heart should occupy approximately 1/3 rd of the chest and seen such that ''3 hearts'' could fit into the thorax.
3. Function: in the transthoracic four-chamber view,both ventricles should squeeze vigorously and equally toward the ventricular septum, such that the heart does not appear to ''rock'' within the chest.
4. Rhythm: while observing the heart, there should be a relatively steady rate within the range of 120-180 beats per minute without early beats, blocked beats,or periods of bradycardia or tachycardia.
5. Proportion: pairs of cardiac chamber structures should be seen as approximately the same size, right to left, including the atria, ventricles, atrio-ventricular (AV) valves, semilunar valves, great vessels and the SVC and IVC (2).
Colour-flow mapping is an important adjunct to crosssectional scanning and can considerably speed up the cardiac evaluation.The correct direction of flow throughout the cardiac chambers and arch vessels can be demonstrated. It can be used to exclude regurgitation at any valve. At the usual Nyquist limits, unaliased colour flow throughout the heart indicates that the flow is at normal velocities. If colour shows aliasing at any point in the heart, pulsed Doppler should be used to obtain an accurate velocity. The peak velocity at the atrioventricular valves is 30-60 cm/sec and is fairly constant throughout gestation. The peak velocity of flow at the arterial valves is approximately 25 cm/sec at 12 weeks, increasing to 60-100 cm/sec by term. Turning on color flow when the ultrasound beam is perpendicular to the ventricular septum helps to exclude a significant ventricular septal defect [1]. M-mode echocardiography is useful in assessing ventricular function and detecting cardiac rhythm abnormalities [1].
Summary
The foetal echocardiogram is a unique ultrasound examination, which differs from the antenatal obstetrical ultrasound and from the conventional echocardiogram in the infant, child, or adult. A unique, high level set of skills and knowledge is required in order to perform this test. A thorough familiarity with the features of the normal heart is essential in order to detect abnormalities.
References
- L Allan (2004) Technique of Fetal Echocardiography. Pediatr Cardiol 25: 223-233.
- Jack R, Nancy A, Bettina C, Gotteiner N, Hornberger L, et al. (2004) American Society of Echocardiography Guidelines and Standards for Performance of the Fetal Echocardiogram. J Am Soc Echocardiogr 17: 803-810.
- Timothy MC, Patrick WOL, James BS, Hagler DJ (1994) Distinguishing Right from Left: A Standardised Technique for Fetal Echocardiography. J Am Soc Echocardiogr 7: 47-53.
- Dennis W, Maria R-L, Bienvenido P, Weiner S, World Association of Perinatal Medicine Ultrasonography Working Group (2009) Perinatal echocardiography: protocols for evaluating the fetal and neonatal heart. J Perinat Med 37: 5-11.
- Mi-Young L, Hye-Soung W (2013) Technique of fetal echocardiography. Obstet Gynecol Sci 56: 217-226.
INDEXING
PARTNERS









Table 1: Indications for foetal echocardiography. View Table 1